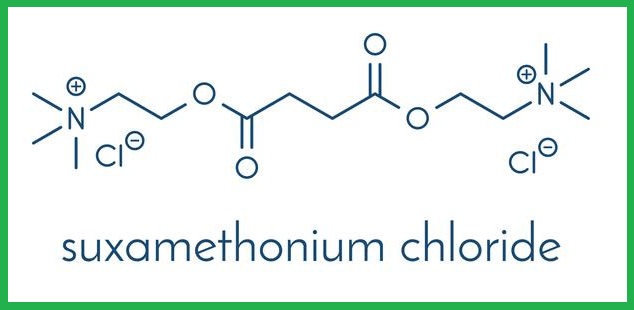
During the last five decades, succinylcholine has been used in clinical practice. It is a potent neuromuscular blocking agent that is widely used in a wide variety of situations. Although succinylcholine has proven to be effective, it is also associated with some serious adverse effects. In addition to prolonging apnea, this drug has been associated with cardiac arrest and hypertension.
In one case of prolonged apnea after administration of succinylcholine, the patient was treated with topical organophosphate anticholinesterase. However, the patient remained apneic for three hours after administering succinylcholine at 0.3 mg/kg. The patient regained spontaneous breathing after three hours and was subsequently managed with elective ventilation. A comprehensive preanaesthetic anamnesis and thorough physical examination are important in identifying developmental delays and other factors that may be causing the patient’s apnea.
The mechanism by which succinylcholine prolongs apnea is not fully understood.
Possible causes include a marked deficiency of pseudocholinesterase, organophosphate toxicity, and low serum cholinesterase activity caused by organophosphates. In some cases, the rate of cholinesterase activity is decreased due to severe renal or liver failure. In others, the process is prolonged in patients with atypical plasma cholinesterase. Atypical plasma cholinesterase is not found in the normal population and can be a result of genetic or acquired disorders.
In a study by Foldes and colleagues, a case of prolonged apnea following administration of succinylcholine was described. The patient was a 53-year-old woman with a history of suicidal attempt by organophosphate pesticide poisoning. She was admitted to a tertiary military hospital in India and advised to undergo MECT. She had been on acetaminophen with codeine for trigeminal neuralgia due to repetitive sinus infections. She had a previous episode of apnea after the Caldwell-Luc procedure in 1981. She had also been on a continuous dose of propofol in combination with intermittent doses of morphine.
In this case, a detailed history and physical examination were performed and the patient’s respiratory status was assessed by ABG. After complete muscle paralysis, the patient was given MECT by a psychiatrist. She was then oxygenated with bag and mask ventilation. After a few minutes of respiration, the first twitch was noticed. The patient’s condition was stabilized and she was discharged. During the following week, she underwent multiple consultations with a psychotherapist for probable mental illness. The patient was monitored for a period of more than seven hours and was discharged with continued ventilatory support.
Succinylcholine has been shown to be contraindicated in patients with skeletal muscle myopathy, rhabdomyolysis, or malignant hyperthermia. It also has the potential to cause sudden cardiac arrest and ventricular dysrhythmias. In addition, it has been reported that the incidence of bradycardia is higher in pediatric patients. This is particularly true in the presence of hyperkalemia. In addition, the use of this drug has been associated with an increased risk of sudden cardiac arrest in healthy infants.
While it is common to use neuromuscular blocking agents in emergency situations, a careful history should be taken to identify any signs of development problems or other comorbidities. A detailed preanaesthetic anamnesis is also necessary for any major surgical interventions or other procedures. In the event that the patient develops apnea, an apnea reversal agent must be available. In addition, the patient’s body mass index and ideal body weight should be taken into consideration.