Are you wondering why we take all day looking at what we’re eating and counting calories, keeping track of macros, and stressing over carbohydrates? Yet, we seldom stop to think about what happens in our bodies when we take that first bite. The truth is that it takes place. It’s like the complex chemical reaction that starts at the point food touches your stomach.
That’s where GLP and GIP hormones come into the picture. And honestly? They’re kind of fascinating once you get to know them.
I’ll admit, when I first heard about these two, my eyes glazed over. Acronyms, medical jargon, the whole nine yards. However, the deeper I looked into the functions of GLP as well as GIP hormones, I came to realize that they’re the unspoken behind-the-scenes crew of our metabolism and are constantly working to keep blood sugar under control, as well as our appetite under control and energy levels balanced. Let’s take a moment to look into these biochemical powerhouses, will we?
What Are GLP and GIP Hormones, Anyway?
This is the truth: the gut knows more than you realize. It’s much more than a simple tube that processes food. It’s an endocrine organ that is sophisticated, constantly in contact with your pancreas and brain, and basically all other things. It’s the two top players? GLP as well as GIP.
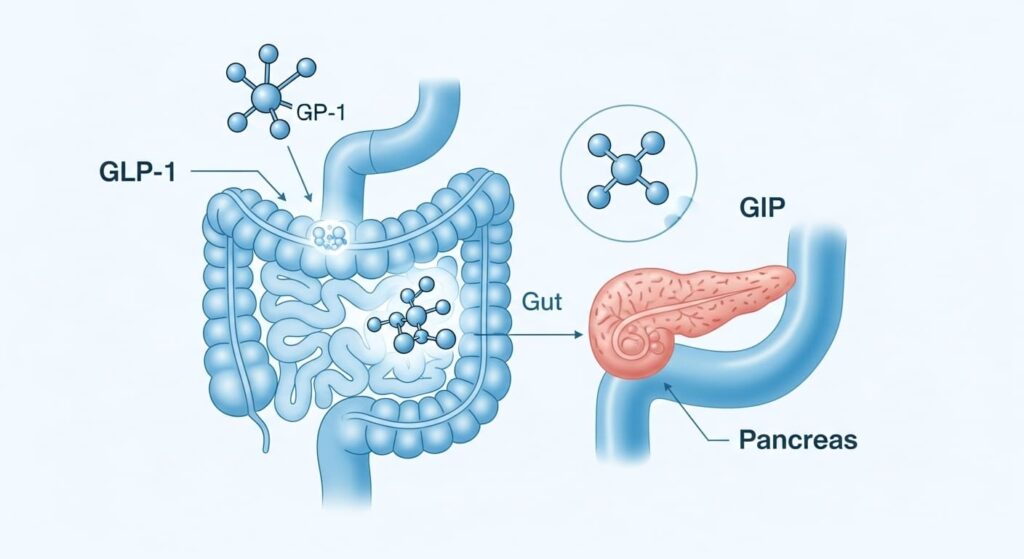
GLP is a short form for Glucagon-Like Peptide-1 (we often call it GLP-1 for simplicity). GLP stands for Glucagon-Like Peptide-1, while GIP is a shorthand for Glucose-dependent Insulinotropic Polypeptide. It’s quite a mouthful. GIP was originally known as Gastric Inhibitory Polypeptide, but researchers changed the name because they recognized that GIP does more than simply inhibit gastric stuff.
Both of these hormones belong to a family called incretins. Think of incretins as chemical messengers that get released from your intestines when you eat, especially when there’s glucose in the mix. Their main job? To tell your pancreas, “Hey, insulin time! We’ve got incoming sugar to deal with.
What I find remarkable is that these hormones are glucose-dependent. They only really kick into high gear when blood sugar is elevated. It’s like they have this built-in safety mechanism that prevents your blood sugar or glucose from dropping too low. Pretty clever design, if you ask me.
The GLP Hormone Role: More Than Just Insulin
Let’s talk about GLP-1 first. This hormone is secreted mainly by L-cells in your small intestine and colon. The moment food, especially carbohydrates and fats, enters your gut, these cells spring into action.
GLP and GIP function in overlapping but distinct ways, and GLP-1 has some particularly interesting tricks up its sleeve. Yes, it stimulates insulin secretion when glucose levels are high. But it also:
- Slows down gastric emptying. Ever wondered why you feel fuller longer after certain meals? Part of that might be GLP-1 telling your stomach to pump the brakes, keeping food in there a bit longer.
- Suppresses glucagon. Glucagon is insulin’s opposite; it raises blood sugar. GLP-1 keeps it in check when you don’t need it.
- Reduces appetite. This is the big one that’s caught everyone’s attention lately. GLP-1 acts on receptors in your brain that influence hunger and satiety. It’s why drugs that mimic GLP-1 have become game-changers for weight loss.
I’ve always wondered why some meals leave me satisfied for hours while others have me raiding the fridge an hour later. Turns out, the GLP hormone’s role in appetite regulation is a huge part of that puzzle.
The GIP Hormone Role: The Underappreciated Partner
Now, GIP doesn’t always get the same spotlight as GLP-1, but that doesn’t mean it’s any less important. Secreted by K-cells in the upper part of your small intestine, GIP responds quickly to food intake, especially fats and carbohydrates.
The GIP hormone’s role in glucose metabolism is substantial. Like GLP-1, it enhances insulin secretion in a glucose-dependent manner. However, here’s where things become exciting: GIP also has effects on the fat tissue. In fact, it promotes the storage of fat in Adipocytes (fat cells) when certain conditions are met. Researchers believe that this may be beneficial to evolutionary evolution by being able to store energy effectively in times of food availability. With our current world of continuous food supply, however, it’s more difficult.
Also, there is evidence to suggest that GIP can influence bone metabolism and could even cause adverse cardiovascular consequences. As we continue to study the subject, the more we understand how interconnected these networks really are.
GLP vs GIP: A Comparison Worth Understanding
So, GLP vs GIP, how do they stack up against each other? It’s not really a competition, but understanding their differences helps paint the full picture of the incretin system.
Both are incretins. Both stimulate insulin secretion. Both are degraded by the same enzyme (DPP-4, but we’ll get to that). But their GLP GIP comparison reveals some key distinctions:
Where they’re produced: GLP-1 comes from L-cells in the lower intestine; GIP is produced in K-cells of the upper intestine.
Timing: When food hits your duodenum, GIP will release first before GLP-1 follows soon afterwards as nutrients travel further along your digestive system.
Appetite effects: This is big. GLP-1 clearly suppresses appetite and slows gastric emptying. GIP? Not so much. In fact, some studies suggest GIP might not have the same appetite-suppressing effects, and in some contexts, it might even promote nutrient storage rather than satiety.
Clinical implications: The appetite and weight effects of GLP-1 have made GLP-1 receptor agonists blockbuster drugs. GIP’s role is more nuanced; some newer medications actually combine GLP-1 and GIP agonism (like tirzepatide), which seems to work even better than GLP-1 alone. Who would’ve thought?
On the flip side, some research has explored blocking GIP while increasing GLP-1 production potentially providing metabolic benefits as well. Science continues to evolve at an incredible rate it truly fascinating watching its progress unfold before our very eyes!
GLP and GIP Physiology: The Incretin System Explained
Alright, let’s zoom out and look at the bigger picture: GLP and GIP physiology within what’s called the incretin system.
Here’s a wild fact: when you eat something and your blood glucose/ sugar rises, your pancreas releases insulin to handle it. But wait here is where things become interesting: insulin release is actually stronger when glucose comes from food rather than when you inject an equivalent amount directly into your bloodstream, something known as the “incretin effect.” Scientists refer to this phenomenon.
Why? Because of GLP and GIP hormones. They amplify the insulin response. It’s like they’re turning up the volume on your pancreas’s signal.
- You eat food containing carbohydrates and fats.
- As nutrients enter your gut, K-cells release GIP (quickly), and L-cells release GLP-1 (a bit later).
- These hormones travel through your bloodstream to your pancreas.
- They bind to receptors on beta cells (the insulin-producing cells).
- This binding enhances glucose-stimulated insulin secretion, but only when blood sugar is elevated.
- Insulin does its job: shuttling glucose into cells, lowering blood sugar.
- Meanwhile, GLP-1 also slows gastric emptying and signals your brain that you’re satisfied.
The GLP and GIP incretin system explained goes something like this:
The beauty of the GIP and GLP mechanism is that it’s self-regulating. When blood sugar drops back to normal, the incretin effect diminishes. Your body doesn’t overshoot and cause hypoglycemia (low blood sugar) under normal circumstances.
But here’s the fragile part: both GLP-1 and GIP are rapidly broken down by an enzyme called DPP-4 (dipeptidyl peptidase-4). Their half-lives are just a couple of minutes. Blink, and they’re gone. This is actually why many diabetes medications either mimic these hormones in a DPP-4-resistant form or block the DPP-4 enzyme itself to let natural GLP-1 and GIP hang around longer.
Why This Matters More Than You Think
GLP and GIP function has revolutionized my perceptions of metabolism, weight control and hunger management. They’re not simply abstract concepts in biology textbooks – these molecules play an essential part in daily dining experiences which leave us satisfied while conserving energy reserves.When the incretin system works well, blood sugar remains balanced.. Appetite is regulated. Your pancreas isn’t overworked. But when things go awry, as they can in type 2 diabetes, the incretin effect is often reduced. That’s partly why medications targeting this system have been so revolutionary.
It’s also why I find myself paying more attention to how I eat, not just what I eat. Eating slowly, for instance, might give those L-cells and K-cells more time to do their thing. Combining protein, fat, and fiber might trigger a more robust incretin response. These are small things, but they add up.
The Takeaway
However, here’s where things become exciting: GIP also has effects on the fat tissue. In fact, it promotes the storage of fat in Adipocytes (fat cells) when certain conditions are met. Researchers believe that this may be beneficial to evolutionary evolution by being able to store energy effectively in times of food availability. With our current world of continuous food supply, however, it’s more difficult.
It’s at the heart of some of the most exciting medical advances in metabolic health, obesity treatment, and diabetes management. And yet, for most of us, these hormones are doing their quiet work every single day, every single meal, without us ever thinking about them.
Maybe that’s the beautiful part. Our bodies are constantly orchestrating this complex symphony of signals and responses, and most of the time, we don’t have to conduct. We just have to show up, eat reasonably well, and trust the process.
But it doesn’t hurt to appreciate the players in the orchestra, does it?
Next time you sit down for a meal, maybe take a moment to think about those incretin hormones gearing up for action. Also, there is evidence to suggest that GIP can influence bone metabolism and could even cause adverse cardiovascular consequences. As we continue to study the subject, the more we understand how interconnected these networks really are.